NMC Royal Hospital Sharjah diagnoses hidden surgical condition behind severe vomiting after semaglutide

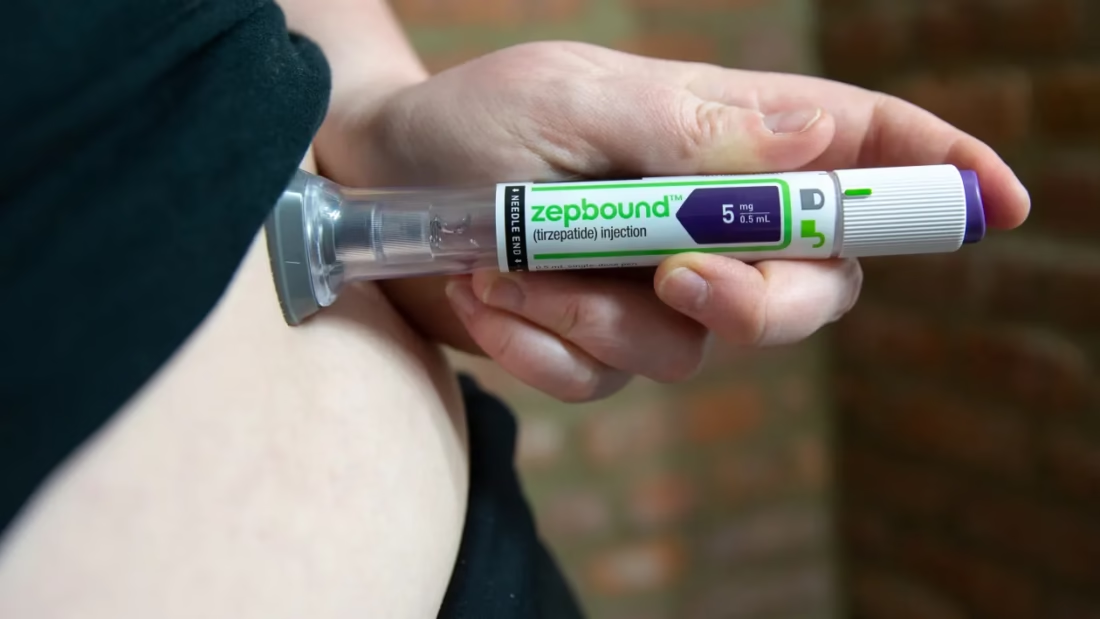
Sharjah: Doctors at NMC Royal Hospital Sharjah have successfully diagnosed and treated a rare congenital surgical condition in a 55-year-old man whose severe vomiting and rapid weight loss worsened after starting semaglutide, highlighting an important message for both clinicians and patients in the era of widely used diabetes and weight-management medications.
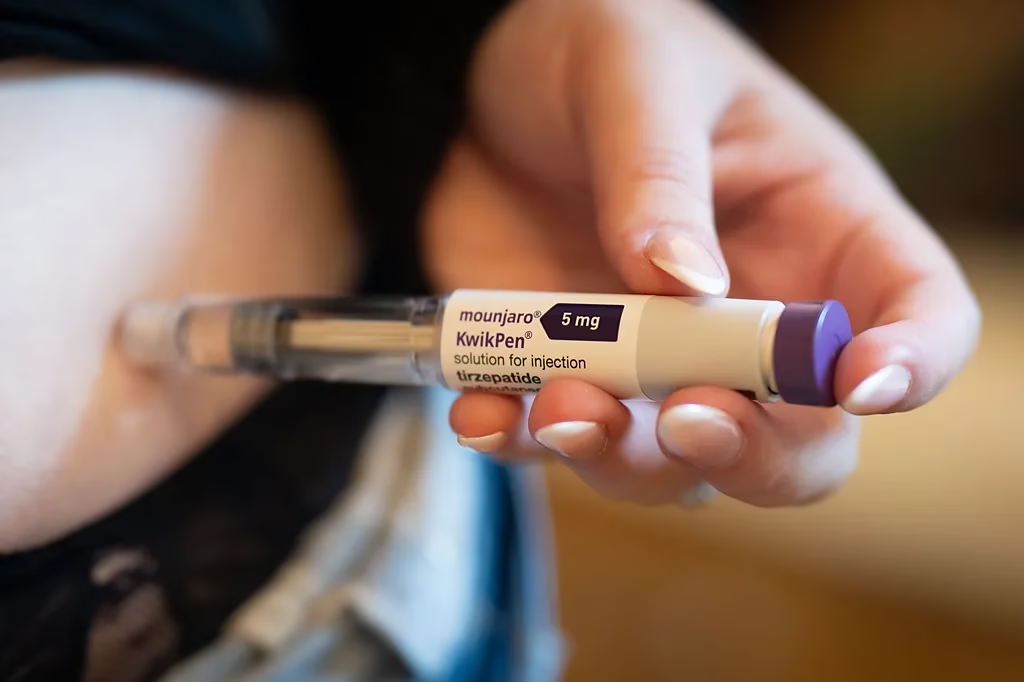
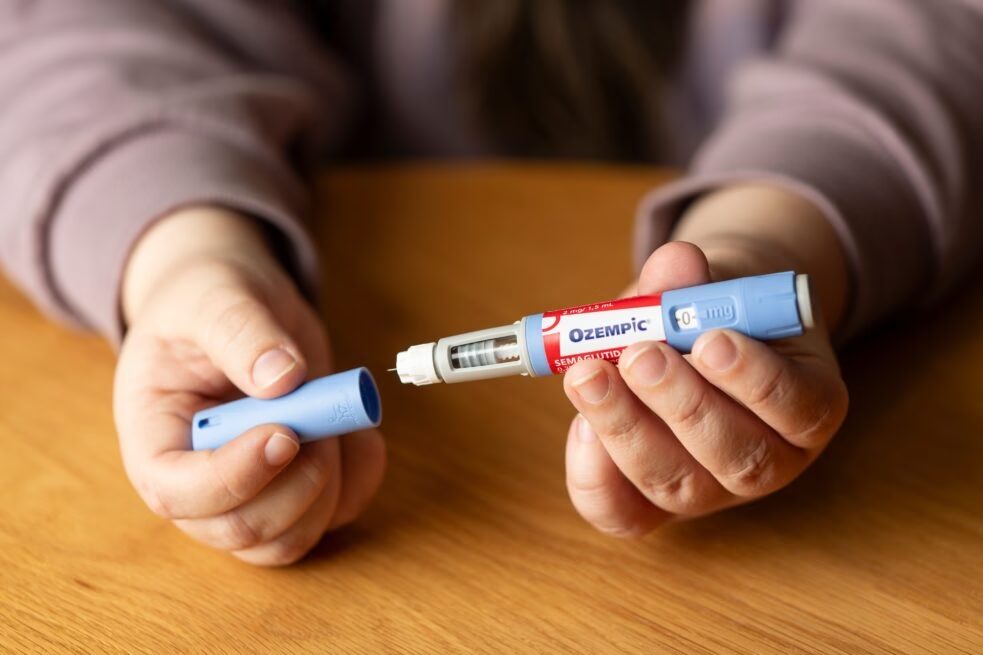
The patient, who had type 2 diabetes mellitus and was already on metformin, began experiencing progressive vomiting after meals over several months, along with significant unintentional weight loss. His symptoms became markedly worse shortly after the introduction of semaglutide, a GLP-1 receptor agonist commonly prescribed to improve blood sugar control and support weight reduction.
Because nausea, appetite suppression and weight loss are known side effects of semaglutide and similar medications, the patient’s condition could easily have been attributed to the drug alone. However, the severity and persistence of his symptoms prompted doctors at NMC Royal Hospital Sharjah to investigate further for an underlying structural cause.
Detailed imaging and diagnostic evaluation revealed that the patient had a partial annular pancreas, a rare congenital abnormality in which pancreatic tissue partially surrounds the duodenum. In this case, the condition had caused narrowing in the second part of the duodenum, resulting in gastric outlet obstruction and preventing food from passing normally from the stomach into the small intestine. He was also found to have symptomatic cholelithiasis, or gallstones.
Given the overlap between expected medication side effects and the patient’s worsening gastrointestinal symptoms, the case presented a significant diagnostic challenge. The medical team carried out extensive investigations, including CT scan, MRI, endoscopic ultrasound, duodenal biopsy, and repeated tumour marker testing, to rule out malignancy. These tests showed no evidence of cancer, despite initial concern due to the nature of the obstruction and the patient’s weight loss.
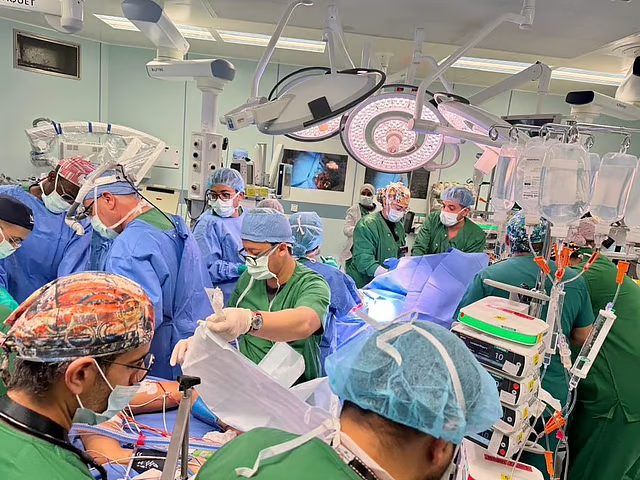
The case was managed by Dr Solomon John, Consultant Surgeon at NMC Royal Hospital Sharjah, who led the surgical team in planning a definitive intervention after the patient’s symptoms remained debilitating.
During surgery, doctors found a dilated first part of the duodenum transitioning to a narrowed second segment encircled by pancreatic tissue, confirming the diagnosis of annular pancreas. Importantly, no visible mass or metastatic deposits were identified. To avoid unnecessary radical surgery, the team performed an intraoperative frozen section biopsy, which confirmed that the tissue was benign.
With cancer excluded, the surgeons were able to avoid a pancreaticoduodenectomy (Whipple procedure) and instead proceed with a more appropriate and organ-preserving treatment. The patient underwent a Roux-en-Y gastrojejunostomy with jejunojejunostomy to bypass the obstruction, along with cholecystectomy to remove the gallbladder. Final pathology later confirmed benign pancreatic tissue with chronic fibrosis.
The patient’s postoperative recovery was uncomplicated. He gradually resumed oral intake, tolerated his diet well, and was discharged with scheduled follow-up.
Commenting on the case, Dr Solomon John, Consultant Surgeon at NMC Royal Hospital Sharjah, said:
“This case is a timely reminder that not every gastrointestinal symptom in patients taking GLP-1 receptor agonists should be assumed to be a routine medication side effect. When vomiting, weight loss, or upper gastrointestinal symptoms are severe or persistent, clinicians should investigate further to rule out an underlying structural problem. In this case, thorough evaluation and timely surgery allowed us to identify the true cause, avoid unnecessary radical resection, and provide the patient with the right treatment.”
This rare case also reflects an increasingly relevant issue in modern clinical practice. As GLP-1 receptor agonists such as semaglutide become more widely used in the management of both diabetes and obesity, physicians may encounter situations where these medications appear to intensify previously silent gastrointestinal conditions. Because GLP-1 therapies naturally delay gastric emptying, they may worsen symptoms in patients with an undiagnosed fixed anatomical obstruction, bringing an underlying disorder to clinical attention.
Doctors say the broader lesson is clear: persistent vomiting, severe digestive symptoms, or unexplained weight loss in patients taking these medications should not automatically be dismissed as expected side effects without proper investigation. Early diagnosis can uncover hidden disease, prevent malnutrition and complications, and ensure patients receive the most appropriate treatment at the right time.
The successful management of this case at NMC Royal Hospital Sharjah highlights the importance of a multidisciplinary approach, involving surgeons, gastroenterologists, radiologists and endocrinologists in evaluating complex presentations and guiding safe, individualized treatment decisions.

 English
English